-
Články
Top novinky
Reklama- Vzdělávání
- Časopisy
Top články
Nové číslo
- Témata
Top novinky
Reklama- Videa
- Podcasty
Nové podcasty
Reklama- Kariéra
Doporučené pozice
Reklama- Praxe
Top novinky
ReklamaFollicular Dendritic Cell-Specific Prion Protein (PrP) Expression Alone Is Sufficient to Sustain Prion Infection in the Spleen
Prion diseases are characterised by the accumulation of PrPSc, an abnormally folded isoform of the cellular prion protein (PrPC), in affected tissues. Following peripheral exposure high levels of prion-specific PrPSc accumulate first upon follicular dendritic cells (FDC) in lymphoid tissues before spreading to the CNS. Expression of PrPC is mandatory for cells to sustain prion infection and FDC appear to express high levels. However, whether FDC actively replicate prions or simply acquire them from other infected cells is uncertain. In the attempts to-date to establish the role of FDC in prion pathogenesis it was not possible to dissociate the Prnp expression of FDC from that of the nervous system and all other non-haematopoietic lineages. This is important as FDC may simply acquire prions after synthesis by other infected cells. To establish the role of FDC in prion pathogenesis transgenic mice were created in which PrPC expression was specifically “switched on” or “off” only on FDC. We show that PrPC-expression only on FDC is sufficient to sustain prion replication in the spleen. Furthermore, prion replication is blocked in the spleen when PrPC-expression is specifically ablated only on FDC. These data definitively demonstrate that FDC are the essential sites of prion replication in lymphoid tissues. The demonstration that Prnp-ablation only on FDC blocked splenic prion accumulation without apparent consequences for FDC status represents a novel opportunity to prevent neuroinvasion by modulation of PrPC expression on FDC.
Published in the journal: . PLoS Pathog 7(12): e32767. doi:10.1371/journal.ppat.1002402
Category: Research Article
doi: https://doi.org/10.1371/journal.ppat.1002402Summary
Prion diseases are characterised by the accumulation of PrPSc, an abnormally folded isoform of the cellular prion protein (PrPC), in affected tissues. Following peripheral exposure high levels of prion-specific PrPSc accumulate first upon follicular dendritic cells (FDC) in lymphoid tissues before spreading to the CNS. Expression of PrPC is mandatory for cells to sustain prion infection and FDC appear to express high levels. However, whether FDC actively replicate prions or simply acquire them from other infected cells is uncertain. In the attempts to-date to establish the role of FDC in prion pathogenesis it was not possible to dissociate the Prnp expression of FDC from that of the nervous system and all other non-haematopoietic lineages. This is important as FDC may simply acquire prions after synthesis by other infected cells. To establish the role of FDC in prion pathogenesis transgenic mice were created in which PrPC expression was specifically “switched on” or “off” only on FDC. We show that PrPC-expression only on FDC is sufficient to sustain prion replication in the spleen. Furthermore, prion replication is blocked in the spleen when PrPC-expression is specifically ablated only on FDC. These data definitively demonstrate that FDC are the essential sites of prion replication in lymphoid tissues. The demonstration that Prnp-ablation only on FDC blocked splenic prion accumulation without apparent consequences for FDC status represents a novel opportunity to prevent neuroinvasion by modulation of PrPC expression on FDC.
Introduction
Prion diseases (Transmissible spongiform encephalopathies; TSE) are sub-acute neurodegenerative diseases that affect both humans and animals. Many prion diseases, including natural sheep scrapie, bovine spongiform encephalopathy, chronic wasting disease in mule deer and elk, and kuru and variant Creutzfeldt-Jakob disease in humans, are acquired by peripheral exposure (eg: orally or via lesions to skin or mucous membranes). After peripheral exposure prions accumulate first upon follicular dendritic cells (FDC) as they make their journey from the site of infection to the CNS (a process termed, neuroinvasion) [1]–[7]. FDC are a unique subset of stromal cells resident within the primary B cell follicles and germinal centres of lymphoid tissues [8]. Prion accumulation upon FDC is critical for efficient disease pathogenesis as in their absence neuroinvasion are impaired [1]–[4]. From the lymphoid tissues prions invade the CNS via the peripheral nervous system [9].
During prion disease aggregations of PrPSc, an abnormally folded isoform of the cellular prion protein (PrPC) accumulate in affected tissues. Prion infectivity co-purifies with PrPSc [10] and is considered to constitute the major, if not sole, component of infectious agent [11]. Host cells must express cellular PrPC to sustain prion infection [12] and FDC appear to express high levels of PrPC on the cell membrane in uninfected mice [13], [14]. Although prion neuroinvasion from peripheral sites of exposure is dependent upon the presence of FDC in lymphoid tissues, it is not known whether FDC actually replicate prions themselves. FDC characteristically trap and retain native antigen on their surfaces for long periods in the form of immune complexes, consisting of antigen-antibody and/or complement components. Prions are also considered to be acquired by FDC as complement-opsonized immune complexes [15]–[18]. Thus, during prion infection FDC might simply trap and retain PrPSc-containing immune complexes on their surfaces following synthesis by other infected cells such as neurones.
Many cell types including classical DC, lymphocytes, mast cells, platelets, reticulocytes and epithelial cells secrete membrane vesicles termed exosomes that are enriched in cell-specific protein [19], [20]. Although the functions of exosomes are uncertain FDC can bind them on their surfaces. These microvesicles permit FDC to passively acquire and display proteins on their surfaces that they do not express at the mRNA level [21]. Studies have shown that prions only accumulated in the spleens of mice in which the FDC-containing stromal compartment expressed PrPC [13], [14]. However, in each of those studies it was not possible to dissociate the Prnp expression status of the FDC from that of the nervous system and all other host-derived non-haematopoietic and stromal cell populations [13], [14], [22]. This is important as prion infection can occur within inflammatory PrPC-expressing stromal cells that are distinct from FDC [23]. Furthermore, as both PrPC and PrPSc can be released from cells in association with exosomes [20] FDC may passively acquire PrPC and prions after release in exosomes from other infected cells [24], [25].
No therapies are available to treat prions diseases. A thorough characterization of the host cells that are infected by prions is imperative for the identification of candidate molecular targets for therapeutic intervention, the development of useful pre-clinical diagnostics and to aid our understanding of the risk of transmission. To definitively determine the role of FDC in prion pathogenesis, two unique compound transgenic mouse models were created in which PrPC expression was specifically “switched on” or “switched off” only on FDC. These mice were then used to establish: i) whether FDC express PrPC or simply acquire it from other host cells; and ii) whether FDC amplify prions, or simply acquire them from other infected host cells. Our data clearly show that PrPC-expressing FDC alone are sufficient to sustain prion replication in the spleen. Furthermore, prion replication in the spleen is blocked in mice in which PrPC-expression is specifically ablated only on FDC.
Results
Mice expressing Cre recombinase specifically in FDC
To study FDC-specific gene function transgenic mice were used that expressed Cre recombinase under the control of the Cr2 locus (CD21-Cre mice) which directs expression in FDC and mature B cells [26], [27]. First the cellular specificity of the Cre recombination was assessed by crossing the CD21-Cre mice with the ROSA26flox/flox reporter strain [28]. Histological analysis showed efficient LacZ expression indicative of Cre-mediated gene recombination in FDC and B cell follicles in the spleens, lymph nodes and Peyer's patches of CD21-Cre ROSA26flox/flox mice (Figure 1A, B). No recombination was observed in FDC and mature B cells in the spleens of ROSA26flox/flox reporter mice that lacked Cre expression (Figure 1B). Unlike lymphocytes, FDC do not derive from bone marrow precursors [29]. As a consequence, it is possible to mix-and-match the genotype of FDC and lymphocytes by grafting bone marrow cells from donor mice into recipients of a different genetic background [13], [14], [22]. To restrict Cre-expression to FDC, adult CD21-Cre ROSA26flox/flox mice were lethally γ-irradiated and 24 h later reconstituted with bone marrow from Cre-deficient C57BL/6 wild-type (WT) mice (termed WT→CD21-Cre ROSA26flox/flox mice) and tissues from six mice from each group analysed 100 days after transfusion. Using this approach, in these mice all B cells lack Cre-expression as they derive from the WT donor bone marrow, whereas the FDC express Cre as they are host-derived. Analysis of the cellular sites of LacZ expression in WT→CD21-Cre ROSA26flox/flox mice confirmed that Cre-mediated recombination was associated with FDC (Figure 1B). No other cellular sites of Cre-mediated recombination were observed in the spleens of WT→CD21-Cre ROSA26flox/flox mice. Furthermore, no other cellular sites of Cre-mediated recombination were observed in a wide range of non-lymphoid peripheral tissues from CD21-Cre ROSA26flox/flox and WT→CD21-Cre ROSA26flox/flox (heart, liver, kidney, pancreas, ear, tongue, skeletal, muscle, ovary, uterus, bladder, testes, epididymis, sciatic nerve and spinal cord; data not shown). These data clearly demonstrate that CD21-Cre mice are a useful tool to study FDC-specific gene expression and function.
Fig. 1. Cre-mediated gene recombination in FDC in the spleens, lymph nodes and Peyer's patches of CD21-Cre ROSA26flox/Flox mice. 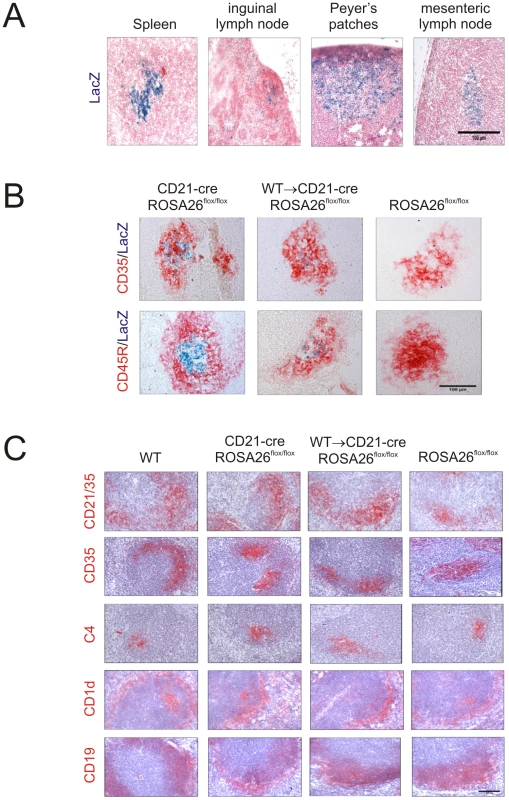
A) Analysis of the cellular sites of LacZ expression (blue) in the spleens, inguinal lymph nodes, Peyer's patches and mesenteric lymph nodes of CD21-Cre ROSA26flox/flox mice shows Cre-mediated recombination in a focus of cells within the B cell follicles. Sections were counterstained with nuclear fast red (red). B) IHC analysis of FDC (CD35+ cells, upper row, red) and B cells (CD45R+ cells, lower row, red) confirmed that Cre-mediated LacZ expression (blue) was associated with FDC in the spleens of WT→CD21-Cre ROSA26flox/flox mice. No LacZ expression was associated with FDC in spleens from ROSA26flox/flox mice that lacked Cre. C) IHC analysis of the status of FDC (CD35+ and C4-binding cells; red) and B cells expressing CD45R, CD19, and CD1d (red) in spleens from WT, CD21-Cre ROSA26flox/flox, WT→CD21-Cre ROSA26flox/flox and ROSA26flox/flox mice. Scale bars 100 µm. n = 6 mice/group. Expression of Cre recombinase by the Cr2 promoter is not toxic to FDC
Cre toxicity can occur in some Cre transgenic mouse lines whereby Cre recombinase causes mis-recombination, DNA damage and death of Cre-expressing cells [30]. However, immunohistochemical (IHC) analysis of spleens from CD21-Cre ROSA26flox/flox mice and WT→CD21-Cre ROSA26flox/flox mice showed no significant effect of Cre-expression on the status of FDC networks and B cell follicles when compared to spleens from WT control mice and ROSA26flox/flox mice that lacked Cre expression (Figure 1C). Furthermore, the expression of Cre recombinase under the control of the Cr2 locus had no observable effect on CD21/35 expression (Figure 1C).
FDC express Prnp and do not acquire PrPC from neighbouring cells
Next, mice were created in which Prnp expression (which encodes PrPC) was restricted only to FDC. To do so, CD21-Cre mice were first bred onto a PrPC-deficient (Prnp-/-) background. The resulting CD21-Cre Prnp-/- mice were then crossed with Prnpstop/- mice in which a floxed β-geo stop cassette was inserted into intron 2 of the Prnp gene upstream of exon 3 [31]. In the progeny CD21-Cre Prnpstop/- mice, PrPC is only expressed in cells expressing Cre recombinase (CD21-expressing FDC and mature B cells). To restrict the Prnp-expression to FDC, CD21-Cre Prnpstop/- mice were lethally γ-irradiated and grafted with bone marrow from Cre-deficient Prnpstop/- mice (Prnpstop/-→CD21-Cre Prnpstop/- mice). We also performed bone marrow transfers from CD21-Cre Prnpstop/- donors into CD21-Cre Prnpstop/- recipients (CD21-Cre Prnpstop/-→CD21-Cre Prnpstop/- mice), CD21-Cre Prnpstop/- donors into Cre-deficient Prnpstop/- mice (CD21-Cre Prnpstop/-→Prnpstop/- mice) and Prnp+/- donors into Prnp+/- recipients (Prnp+/-→Prnp+/- mice) as controls (Figure 2A).
Fig. 2. FDC-restricted PrPc expression in the spleens of Prnpstop/-→CD21-Cre Prnpstop/- mice. 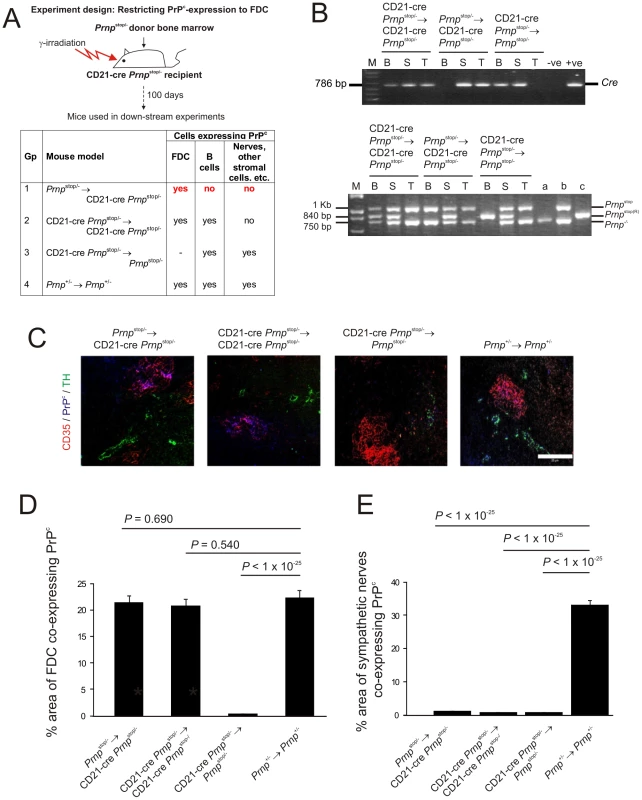
A) The anticipated distribution of PrPC expression on FDC and B cells in tissues from each mouse group. B) The detection of Cre in the tail and spleen but not blood of the Prnpstop/-→CD21-Cre Prnpstop/- mice confirmed the restriction of the Cre-expression to the stromal but not haematopoietic compartments of these mice (upper panel). Efficient Cre-mediated recombination of Prnpstop (Prnpstop(R)) was restricted to the FDC-containing stromal compartment of the spleens of Prnpstop/-→CD21-Cre Prnpstop/- mice when compared to control mice. Cre-mediated recombination by CD21-expressing lymphocytes was efficiently prevented in these mice by the irradiation and transfer of Prnpstop/- bone marrow as demonstrated by the lack of a Prnpstop(R) band in DNA extracted from blood (lower panel). B, blood; S, spleen; T, tail; M, DNA size markers; a, b, c, control DNA samples for each transgene combination tested which were (a) Prnp-/-, (b) Prnpstop/- and (c) complete recombination of the stop cassette within the Prnpstop/- allele. C) IHC analysis of PrPC expression (blue) by FDC (CD35+ cells; red) and sympathetic nerves (TH+ cells, green) confirmed PrPC expression was restricted to FDC in spleens of Prnpstop/-→CD21-Cre Prnpstop/- mice. Scale bar, 100 µm. D) Morphometric analysis confirmed that the magnitude of the PrPC expression co-localized upon the surfaces of FDC in the spleens of Prnpstop/-→CD21-Cre Prnpstop/- mice was similar to that observed upon FDC in spleens from Prnp+/-→Prnp+/- control mice (p<0.690, n = 48 FDC networks/group). In contrast, in the absence of Cre-recombinase expression by FDC in CD21-Cre Prnpstop/-→Prnpstop/- mice, PrPC expression was substantially lower than that observed upon FDC in spleens from Prnp+/-→Prnp+/- control mice (p<1×10-25, n = 48 FDC networks/group). E) Morphometric analysis confirmed that PrPC expression upon the surfaces of sympathetic nerves in the spleens of Prnpstop/-→CD21-Cre Prnpstop/-, CD21-Cre Prnpstop/-→ CD21-Cre Prnpstop/- and CD21-Cre Prnpstop/-→Prnpstop/- mice was significantly ablated when compared to that observed upon sympathetic nerves in spleens from Prnp+/-→Prnp+/- control mice (p<1×10-25, n = 48 sympathetic nerves/group). For all panels n = 6 mice/group. Spleens, tails and blood from six mice from each group were examined 100 days after bone marrow transfusion. PCR analysis of DNA isolated from the tails, blood and spleens of mice in each group was used to confirm the presence of Cre (Figure 2B, upper panel) and Cre-mediated DNA recombination (Figure 2B, lower panel) within the stromal, haematopoietic or both compartments (respectively). The detection of Cre in the tail and spleen but not blood of the Prnpstop/-→CD21-Cre Prnpstop/- mice confirmed the restriction of the Cre-expression to the stromal but not haematopoietic compartments of these mice. In addition, PCR analysis also confirmed that in these mice efficient Cre-mediated recombination of the Prnpstop/- allele was restricted to the FDC-containing stromal compartment of the spleen (Figure 2B). In Prnpstop/-→CD21-Cre Prnpstop/- mice the recombined Prnpstop/- allele (Prnpstop(R)) was detected in the spleen, but not blood and tail. Thus these data indicate that in the spleens of Prnpstop/-→CD21-Cre Prnpstop/- mice Cre-mediated recombination is restricted to FDC and not B cells.
As anticipated, in the spleens of Prnp+/-→Prnp+/- control mice high levels of PrPC expression were observed upon FDC and tyrosine hydroxylase (TH)-positive sympathetic nerves (Figure 2C). In contrast, in the spleens of Prnpstop/-→CD21-Cre Prnpstop/- mice PrPC was only expressed on FDC (Figure 2C). In the absence of Cre-recombinase expression by FDC and peripheral nerves in CD21-Cre Prnpstop/-→Prnpstop/- mice, PrPC expression was not expressed by either cell population (Figure 2C).
Morphometric analysis confirmed that the amount of the PrPC expression co-localized upon the surfaces of FDC in the spleens of Prnpstop/-→CD21-Cre Prnpstop/- mice was not significantly different from that observed upon FDC in spleens from Prnp+/-→Prnp+/- control mice (P<0.69, n = 48 FDC/group; Figure 2D). In contrast, in the absence of Cre-recombinase expression by FDC in CD21-Cre Prnpstop/-→Prnpstop/- mice, PrPC expression was substantially lower than that observed upon FDC in spleens from Prnp+/-→Prnp+/- control mice (P<1×10-25, n = 48; Figure 2D). Morphometric analysis also confirmed that PrPC expression upon the surfaces of sympathetic nerves in the spleens of Prnpstop/-→CD21-Cre Prnpstop/-, CD21-Cre Prnpstop/-→ CD21-Cre Prnpstop/- and CD21-Cre Prnpstop/-→Prnpstop/- mice was significantly ablated when compared to that observed upon sympathetic nerves in spleens from Prnp+/-→Prnp+/- control mice (p<1×10−25, n = 48 sympathetic nerves/group). Together, these data confirm that in the spleens of Prnpstop/-→CD21-Cre Prnpstop/- mice PrPC expression is specifically restricted to FDC, whereas in spleens from CD21-Cre Prnpstop/-→Prnpstop/- mice, FDC lack PrPC expression. FDC can passively acquire the expression of some surface molecules including MHC class II and complement component C4 [21], [32]. However, these data confirm that FDC express high levels of cellular PrPC on their surfaces and do not simply acquire it from neighbouring cells.
IHC analysis confirmed that the microarchitecture (Figure 3A), size (P = 0.755, n = 32; Figure 3B) and number (P = 0.249, n = 32; Figure 3C) of the FDC networks in spleens from mice with Prnp-expression restricted to FDC (Prnpstop/-→CD21-Cre Prnpstop/- mice) were normal when compared to control mice. Other studies have shown that the density of sympathetic nerves can significantly influence the amount of prion accumulation within in the spleen [33]. Quantitative analysis of the relative positioning of FDC and sympathetic nerves showed there were no significant differences in average distance between these cell populations in spleens from each mouse group (Figure 3D & E; P<0.932, n = 48).
Fig. 3. Effect of FDC-restricted PrPc expression on the spleens of Prnpstop/-→CD21-Cre Prnpstop/- mice. 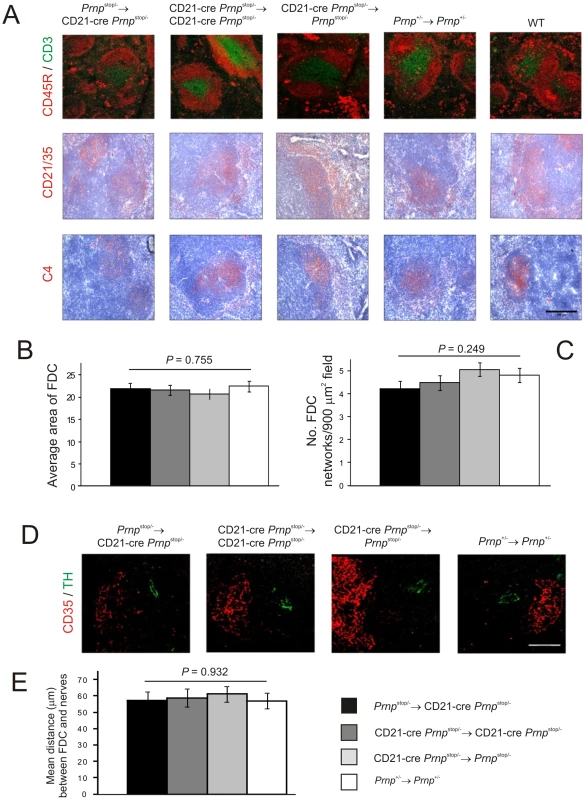
A) IHC analysis of the status of FDC networks (C4-binding cells and CD21/CD35+ cells; red), B cells expressing CD45R (red), and CD3+ T cells (green). Morphometric analysis confirmed that there were no significant difference in the size (B) and number (C) of the CD35+ FDC networks in spleens from Prnpstop/-→CD21-Cre Prnpstop/-, CD21-Cre Prnpstop/-→CD21-Cre Prnpstop/-, CD21-Cre Prnpstop/-→Prnpstop/- mice and Prnp+/-→Prnp+/- control mice (n = 32 FDC networks/group). D and E), Comparison of the sympathetic innervation in spleens from each mouse group. D) IHC detection of TH-positive sympathetic nerves (green) and FDCs (CD35+ cells; red). Scale bar, 50 µm. E) Quantitative analysis of the relative positioning of the FDC and sympathetic nerves showed there were no significant differences in average distance between these cell populations in spleens from each mouse group (P = 0.932, n = 48 FDC networks/group). For all panels n = 6 mice/group. FDC-restricted PrPC-expression is sufficient to sustain prion replication in the spleen
Next, we determined the effect of FDC-restricted Prnp-expression on prion replication in the spleen. In this study, the normal cellular form of the prion protein is referred to as PrPC, and two distinct terms (PrPSc or PrPd) are used to describe the disease-specific, abnormal accumulations of PrP that are characteristically found only in prion-affected tissues and considered a reliable biochemical marker for the presence of infectious prions [10]. Disease-specific PrP (PrPd) accumulations are relatively resistant to proteinase K (PK) digestion, whereas cellular PrPC is destroyed. Where we were able to confirm this resistance by treatment of samples with PK and subsequent paraffin-embedded tissue (PET) immunoblot analysis [34], PrPSc is used as a biochemical marker for the presence of prions. Unfortunately, treatment of tissue sections with PK destroys the microarchitecture. Therefore, for IHC analysis tissue sections were fixed and pre-treated to enhance the detection of the disease-specific abnormal accumulations of PrP (PrPd), whereas cellular PrPC is denatured by these treatments [4]. We have repeatedly shown in a series of studies that these PrPd-accumulations occur only in prion-infected tissues, and correlate closely with the presence of ME7 scrapie prions [1], [4], [13], [35]–[37].
Within weeks after i.p. exposure of WT mice to ME7 scrapie prions, strong accumulations of prion-specific PrPSc occur upon FDCs within the spleen and are sustained until the terminal stages of disease [1], [13], [35]. Here, mice were injected i.p. with ME7 scrapie prions and spleens from 4 mice from each group collected 35, 70 and 105 days after exposure. In spleens from control mice (Prnp+/-→Prnp+/- mice) heavy PrPd accumulations, consistent with localisation upon FDC, were detected at 70 days after i.p. injection with the scrapie agent and had increased in intensity by 105 days after infection (Figure 4A & B). PET immunoblot confirmed the presence of PrPSc upon the surfaces of the FDC in spleens from control mice (Figure 4C). Furthermore, in the spleens of Prnpstop/-→CD21-Cre Prnpstop/- mice in which cellular PrPC was expressed only on FDC, heavy PrPSc accumulations were likewise maintained upon FDC (Figure 4A & B). In contrast, in the absence of PrPC expression by FDC in the spleens of CD21-Cre Prnpstop/-→Prnpstop/- mice, no PrPSc accumulations were observed upon FDC. In the spleens of mice with PrPC-deficient FDC, if PrP was detected at all, it was only occasionally observed within tingible body macrophages (Figure 4A and B, arrowheads; Figure S1). We also analysed prion infectivity levels in spleens collected 70 days after infection from control mice (Prnp+/-→Prnp+/- mice) and Prnpstop/-→CD21-Cre Prnpstop/- mice in which cellular PrPC was expressed only on FDC (Figure S2; n = 3/group). As anticipated high levels of prion infectivity were observed in each control spleen. Furthermore, consistent with data above our analysis showed that PrPc expression only of FDC was sufficient to sustain high levels of prion infectivity within the spleen (Figure S2). These data demonstrate that PrPC expression only on FDC is sufficient to sustain prion replication in the spleen. In the absence of PrPC expression on FDC the prions appeared to be scavenged by tingible body macrophages resident within the B cell follicles.
Fig. 4. Effect of FDC-restricted PrPc expression on PrPSc accumulation in the spleen. 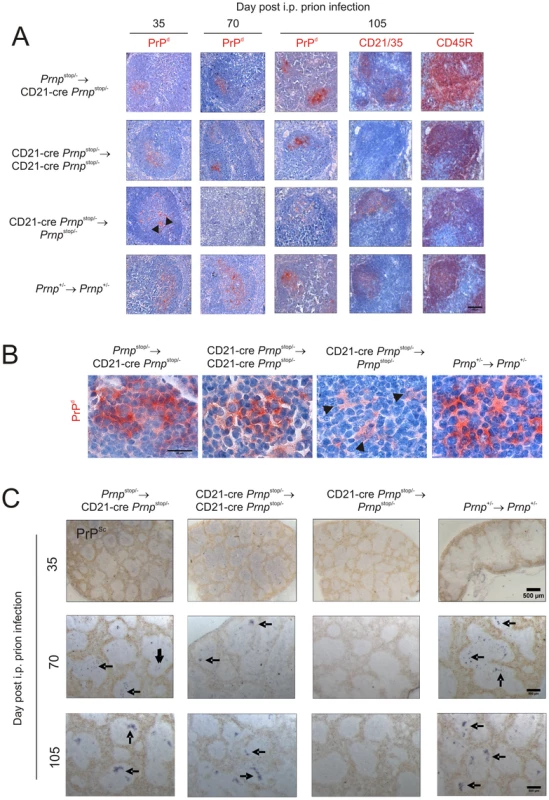
Mice were injected i.p. with the ME7 scrapie agent and tissues collected 35, 70 days and 105 days after exposure. A and B) High levels of PrPd were detected in association with FDC (CD21/35 positive cells) in the B cell follicles (CD45R positive cells) of spleens of mice with PrPC-expressing FDC: Prnpstop/-→CD21-Cre Prnpstop/- mice, CD21-Cre Prnpstop/-→CD21-Cre Prnpstop/- mice and Prnp+/-→Prnp+/- control mice. B) High magnification images of the sites of PrPd accumulation (red) at 70 days post-injection with scrapie. Arrowheads show PrP-accumulation within tingible body macrophages. C) Analysis of adjacent sections by PET-immunoblot analysis confirmed the presence of PK-resistant PrPSc (blue/black). In contrast, no PrPd or PrPSc was detected in spleens of CD21-Cre→Prnpstop/-mice that lacked PrPC-expressing FDC. Arrows indicate PrPSc accumulation upon FDC. A, scale bar = 100 µm. B, scale bar = 20 µm. C, scale bar = 500 µm. For all panels n = 4 mice/group. FDC-specific Prnp-ablation
Next, mice were created in which Prnp expression was specifically ablated in FDC. To do so, CD21-Cre Prnp-/- mice were crossed with mice carrying a “floxed” Prnp gene (Prnpflox/flox mice; [31]). In the progeny CD21-Cre Prnpflox/- mice, Prnp expression is conditionally ablated in cells expressing Cre recombinase (CD21-expressing FDC and mature B cells). To restrict the Prnp-ablation to FDC, CD21-Cre Prnpflox/- mice were lethally γ-irradiated and grafted with bone marrow from Cre-deficient Prnpflox/- mice (Prnpflox/-→CD21-Cre Prnpflox/- mice). We also performed bone marrow transfers from CD21-Cre Prnpflox/- donors into CD21-Cre Prnpflox/- recipients (CD21-Cre Prnpflox/- mice→CD21-Cre Prnpflox/- mice), CD21-Cre Prnpflox/- donors into Cre-deficient Prnpflox/- mice (CD21-Cre Prnpflox/-→Prnpflox/- mice), and Prnp+/- donors into Prnp+/- recipients (Prnp+/-→Prnp+/- mice) as controls (Figure 5A). Spleens, tails and blood from 6 mice from each group were examined 100 days after bone marrow transfusion. PCR analysis of DNA isolated from the spleens, blood and tails of Prnpflox/-→CD21-Cre Prnpflox/- mice confirmed that efficient Cre-mediated DNA recombination and Prnp-ablation was restricted to the FDC-containing stromal compartment of the spleen (Figure 5B). In Prnpflox/-→CD21-Cre Prnpflox/- mice the recombined Prnpstop/- allele (Prnpdeflox) was detected in the spleen, but not blood and tail. Thus these data indicate that in the spleens of Prnpstop/-→CD21-Cre Prnpstop/- mice Cre-mediated recombination and Prnp-ablation is restricted to FDC and not B cells.
Fig. 5. FDC-restricted PrPc-ablation in the spleens of Prnpflox/-→CD21-Cre Prnpflox/- mice. 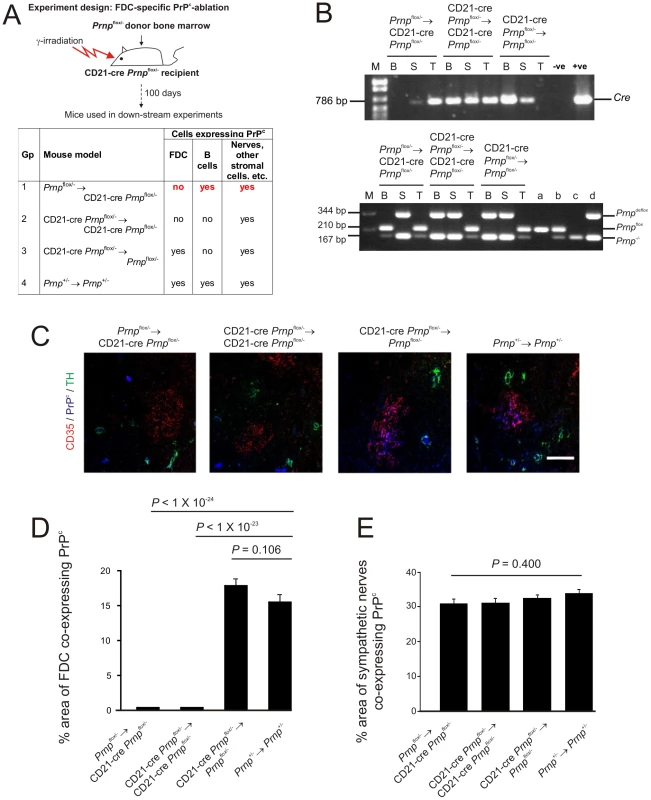
A) The anticipated distribution of PrPC expression on FDC and B cells in tissues from each mouse group. B) PCR analysis of DNA isolated from the spleens, blood and tails of Prnpflox/-→CD21-Cre Prnpflox/- mice confirmed that efficient Cre-mediated DNA recombination and Prnp-ablation (Prnpdeflox) was restricted to the FDC-containing stromal compartment of the spleen. Cre-mediated recombination of CD21-expressing lymphocytes was efficiently prevented in these mice by the irradiation and transfer of Prnpflox/- bone marrow as demonstrated by the lack of a Prnpdeflox band in DNA extracted from blood (lower panel). B, blood; S, spleen; T, tail; M, DNA size markers; a, b, c, d control DNA samples for each transgene combination tested which were (a) Prnpflox/flox,(b) Prnpflox/-, (c) Prnp-/- and (d) Prnpflox/- with complete recombination of the floxed exon 3. C) IHC analysis of PrPC expression (blue) by FDC (CD35+ cells; red) and sympathetic nerves (TH+ cells, green) confirmed the PrPC-ablation was restricted to FDC in spleens of Prnpflox/-→CD21-Cre Prnpflox/- mice. Scale bar, 100 µm. D) Morphometric analysis confirmed that the magnitude of the PrPC expression co-localized upon the surfaces of FDC in the spleens of Prnpflox/-→CD21-Cre Prnpflox/- mice was significantly lower than that observed upon FDC from Prnp+/-→Prnp+/- control mice (P<1.0×10-24, n = 48 FDC networks/group). In contrast, in the absence of Cre-recombinase expression by FDC in CD21-Cre Prnpflox/-→Prnpflox/-mice, PrPC expression was similar to that observed upon FDC in spleens from Prnp+/-→Prnp+/- control mice (P = 0.106, n = 48 FDC networks/group). E) Morphometric analysis confirmed that the magnitude of the PrPC expression co-localized upon the surfaces sympathetic nerves in the spleens of Prnpflox/-→CD21-Cre Prnpflox/-, CD21-Cre Prnpflox/-→ CD21-Cre Prnpflox/- and CD21-Cre Prnpflox/-→Prnpflox/- mice was not significantly different when compared to that observed upon sympathetic nerves in spleens from Prnp+/-→Prnp+/- control mice (p = 0.400, n = 48 sympathetic nerves/group). For all panels n = 6 mice/group. IHC analysis showed that in the spleens of Prnpflox/-→CD21-Cre Prnpflox/- mice and CD21-Cre Prnpflox/- mice→CD21-Cre Prnpflox/- mice FDC did not express PrPC whereas high levels were associated with TH-positive sympathetic nerves (Figure 5C). In the absence of Cre-recombinase expression by FDC in CD21-Cre Prnpflox/-→Prnpflox/- mice, high levels of PrPC were expressed by FDC and sympathetic nerves (Figure 5C).
Morphometric analysis confirmed that the magnitude of the PrPC expression co-localized upon the surfaces of FDC in the spleens of Prnpflox/-→CD21-Cre Prnpflox/- mice and CD21-Cre Prnpflox/- mice→CD21-Cre Prnpflox/- mice was substantially lower than that observed upon FDC in spleens from Prnp+/-→Prnp+/- control mice (P<1×10-24 and P<1×10−23, respectively, n = 48 FDC/group) and not significantly different when compared to background levels (Figure 5D). In contrast, in the absence of Cre-recombinase expression by FDC in CD21-Cre Prnpflox/-→Prnpflox/- mice, PrPC expression was not significantly different from the level observed upon FDC in spleens from Prnp+/-→Prnp+/- control mice (P<0.106; Figure 5D). In contrast, morphometric analysis showed that the magnitude of the PrPC expression co-localized upon the surfaces sympathetic nerves in the spleens of Prnpflox/-→CD21-Cre Prnpflox/-, CD21-Cre Prnpflox/-→ CD21-Cre Prnpflox/- and CD21-Cre Prnpflox/-→Prnpflox/- mice was similar to that observed upon sympathetic nerves in spleens from Prnp+/-→Prnp+/- control mice (p = 0.400, n = 48 sympathetic nerves/group). Together, these data confirm that in the spleens of Prnpflox/-→CD21-Cre Prnpflox/- mice the Prnp ablation is specifically restricted to FDC.
Effect of FDC-specific Prnp-ablation on FDC status and splenic microarchitecture
Data in the current study definitively demonstrate that FDC express high levels of PrPC but the role PrPC plays in FDC function and homeostasis is not known. IHC analysis showed that the microarchitecture of the FDC networks from Prnp-ablated Prnpflox/-→CD21-Cre Prnpflox/- mice were normal when compared to control mice (Figure 6A). Furthermore, no significant difference was observed in the size (P = 0.750, n = 32) and number (P = 0.713, n = 32 of the FDC networks in spleens from each mouse group (Figure 6B & C, respectively). The relative positioning of the FDC and sympathetic nerves was likewise similar in spleens from each mouse group (Figure 6D & E; P<0.765, n = 48).
Fig. 6. Effect of FDC-restricted PrPC-ablation on FDC status. 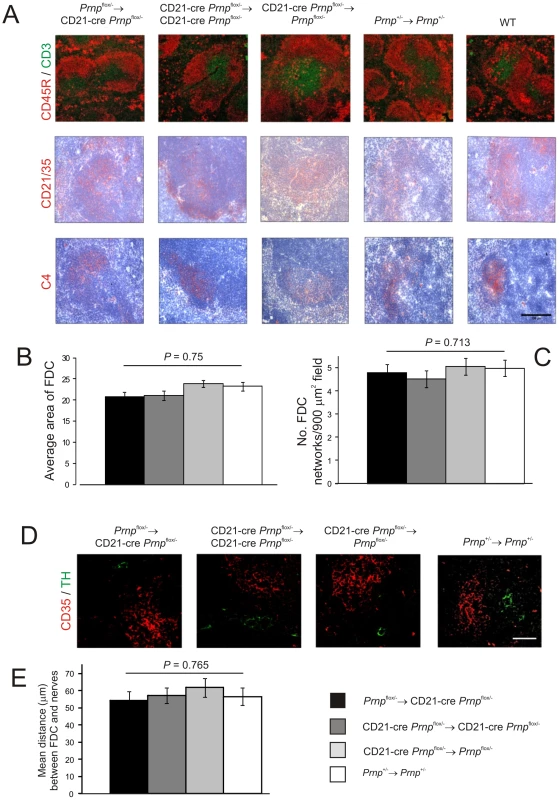
A) IHC analysis of the status of FDC (C4-binding cells and CD21/CD35+ cells; red), B cells expressing CD45R (red), and CD3+ T cells (green). Morphometric analysis confirmed that there were was no significant difference in the size (B) and number (C) of the CD35+ FDC networks in spleens of mice from each mouse group (n = 32 FDC networks/group). D and E), Comparison of the sympathetic innervation in spleens from Prnpflox/-→CD21-Cre Prnpflox/-, CD21-Cre Prnpflox/-→CD21-Cre Prnpflox/-, CD21-Cre Prnpflox/-→Prnpflox/-mice and Prnp+/-→Prnp+/- control mice. D) IHC detection of TH-positive sympathetic nerves (green) and FDCs (CD35+ cells; red). Scale bar, 50 µm. E) Quantitative analysis of the relative positioning of the FDC networks and sympathetic nerves showed there was no significant difference in the average distance between these cell populations in spleens from each mouse group (P = 0.765, n = 48 FDC networks/group). For all panels n = 6 mice/group. FDC characteristically trap and retain native antigen on their surfaces in the form of immune complexes, consisting of antigen-antibody and/or complement components. Antigens trapped on the surface of FDC are considered to promote immunoglobulin-isotype class switching, affinity maturation of naïve IgM+ B cells and the maintenance of immunological memory [38]–[42]. Indeed, prions are also considered to be acquired by FDC as complement-opsonized immune complexes [15]–[18]. To determine whether antigen retention by Prnp-ablated FDC was affected six mice from each group were passively immunized with preformed PAP immune complexes, and 24 h later, the presence of FDC-associated immune complexes identified by IHC (Figure 7) and the presence of peroxidase activity (data not shown). No significant difference in the magnitude of immune complex trapping could be detected between FDC from Prnp-ablated Prnpflox/-→CD21-Cre Prnpflox/- mice and control mice (Figure 7; P = 0.85, n = 40/group). Together, these data demonstrate that Prnp-ablation does not impair FDC status or their ability to trap and retain immune complexes.
Fig. 7. Effect of FDC-restricted PrPC-ablation on immune complex trapping. 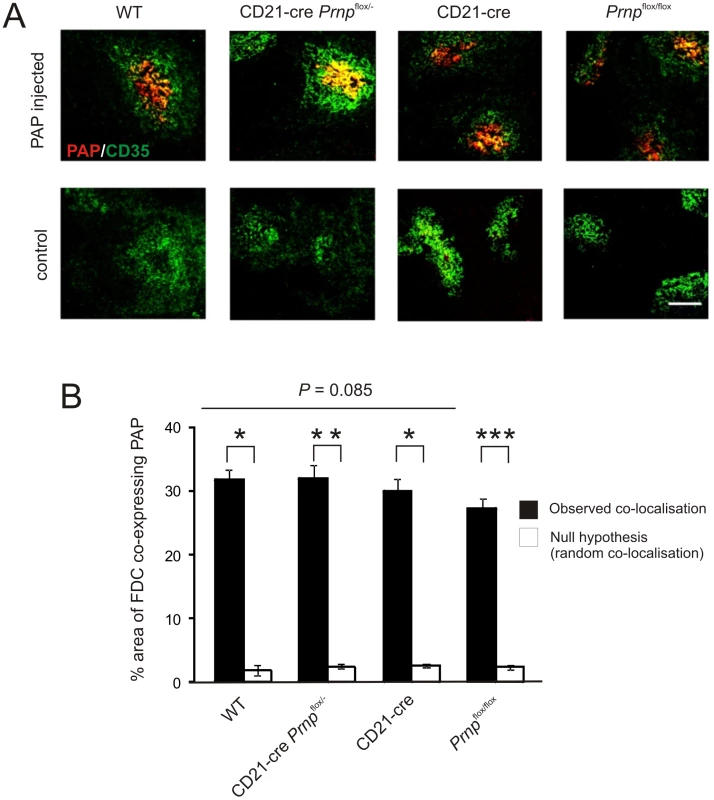
A) Mice were passively immunized with preformed PAP immune complexes, and 24 h later, the presence of immune complexes (red) upon FDC (CD35+ cells, green) assessed by IHC. Scale bar, 100 µm. B) Morphometric analysis confirmed that the magnitude of the immune complex-trapping co-localized upon the surfaces of FDC from Prnp-ablated Prnpflox/-→CD21-Cre Prnpflox/- mice was not significantly different from that observed in spleens from control mice. This analysis also confirmed that the immune complexes were preferentially associated with FDC in these tissues and significantly greater than the null hypothesis that the pixels were randomly distributed. *, P<1×10−21; **, P<1×10−32; *** P<9×10−28; n = 40 FDC networks/group. For all panels n = 6 mice/group. FDC-restricted PrPC-ablation blocks prion replication in the spleen
Next, the effect of FDC-specific Prnp-ablation on prion replication by FDC was determined. Mice were injected i.p. with ME7 scrapie prions and spleens from 4 mice from each group collected 70 days after exposure. As anticipated, heavy PrPd (Figure 8A and B) and PrPSc (Figure 8C) accumulations consistent with localisation upon FDC were detected in spleens from control mice (Prnp+/-→Prnp+/- mice) and mice in which Prnp was ablated only in mature B cells (CD21-Cre Prnpflox/-→Prnpflox/- mice). In the spleens in which cellular PrPC was ablated only on FDC (Prnpflox/-→CD21-Cre Prnpflox/- mice), or FDC and mature B cells (CD21-Cre Prnpflox/-→CD21-Cre Prnpflox/- mice), no PrP accumulations were observed upon FDC (Figure 8A–C). Consistent with data above (Figure 4), in spleens of mice with PrPC-deficient FDC PrP accumulations were only occasionally observed within tingible body macrophages (Figure 8A and B, arrowheads; Figure S1). We also analysed prion infectivity levels in spleens from Prnpflox/-→CD21-Cre Prnpflox/- mice in which cellular PrPC expression was ablated only on FDC (Figure S2; n = 3). Consistent with data above this analysis showed that in the absence of PrPc expression only on FDC the accumulation of high levels of prion infectivity in the spleen was blocked (Figure S2). Taken together, these data show that in the specific absence of PrPC expression FDC are unable to sustain prion replication upon their surfaces and as a consequence the agent is scavenged by tingible body macrophages.
Fig. 8. Effect of FDC-restricted PrPC-ablation on PrPSc accumulation in the spleen. 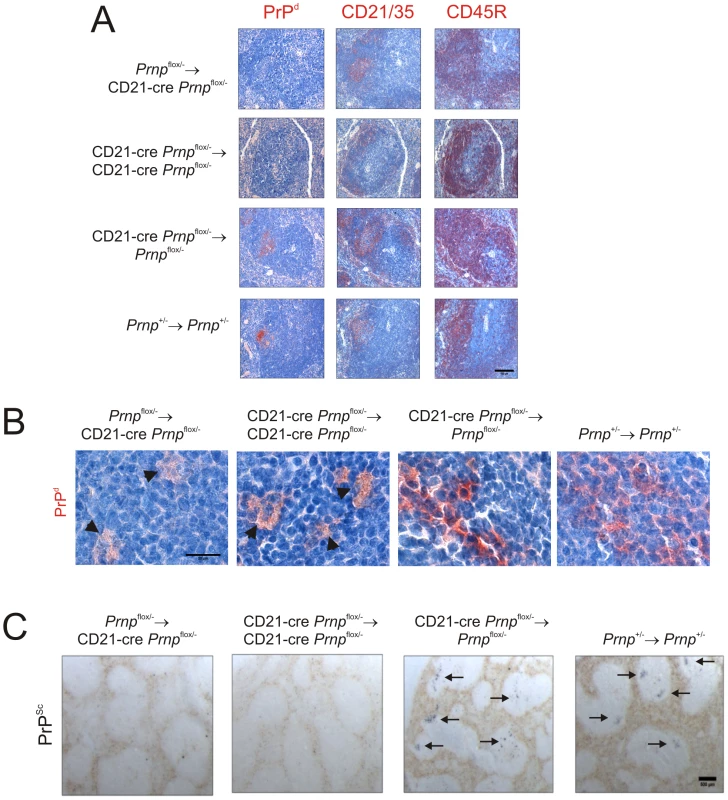
Mice were injected i.p. with the ME7 scrapie agent and tissues collected 70 days after exposure. A) High levels of PrPd (red, left-hand column) were detected in association with FDC (red, middle column) in the B cell follicles (red, right-hand column) of spleens from CD21-Cre Prnpflox/-→Prnpflox/-mice and Prnp+/-→Prnp+/- control mice that contained PrPC-expressing FDC. B) High magnification images of the sites of PrPd accumulation (red) at 70 days post-injection with scrapie. C) PET blot analysis of analysis of adjacent sections by PET-immunoblot analysis confirmed presence of PK-resistant PrPSc (blue/black). In contrast, no PrPSc was detected in spleens of Prnpflox/-→CD21-Cre Prnpflox/- and CD21-Cre Prnpflox/-→CD21-Cre Prnpflox/- mice that lacked PrPC-expressing FDC. In the spleens of some of these mice, low levels of PrPd were occasionally localised within tingible body macrophages (B, arrowheads). A, scale bar = 100 µm. B, scale bar = 20 µm. C, scale bar = 500 µm. Arrows indicate PrPSc accumulation upon FDC. For all panels n = 4 mice/group. FDC-restricted PrPC-ablation does not influence prion disease and susceptibility when infection is established directly within the CNS
When mice with PrPC-ablated FDC (Prnpflox/-→CD21-Cre Prnpflox/- mice) were injected intracerebrally (i.c.) with the ME7 scrapie agent strain directly into the CNS all mice succumbed to clinical signs of scrapie approximately 300 days after exposure with incubation periods indistinguishable from those of Prnp+/- control mice [43] (Prnpflox/-→CD21-Cre Prnpflox/-, 297±4 days, n = 4; Prnp+/-, 290±4 days, n = 5; P = 0.386). Histopathological analysis showed that brains from all clinically-affected mice from each group displayed the characteristic spongiform pathology, astrogliosis, microgliosis and PrPd accumulation typically associated with terminal infection with the ME7 scrapie agent (Figure 9A). Following i.c.-injection with the ME7 scrapie agent, high levels of PrPSc accumulate upon FDC and are maintained for the duration of the incubation period [13](Figure 9B and C). However, FDC are not critical for ME7 scrapie pathogenesis when infection is established directly within the CNS [4], [13], [35], [44]. In the spleens from clinically-scrapie affected mice in which PrPC expression was specifically ablated only on FDC (Prnpflox/-→CD21-Cre Prnpflox/- mice), PrPSc replication upon FDC was also blocked. These data how that FDC do not simply trap and retain prions after their release from infected neurones in the CNS. These data also confirm that the Prnp-ablation in Prnpflox/-→CD21-Cre Prnpflox/- mice was specific to FDC and had no effect on prion neuropathogenesis and disease susceptibility when the infection was established directly in the CNS.
Fig. 9. Effect of FDC-restricted PrPC-ablation on PrPSc accumulation in the brains and spleens of scrapie-affected mice. 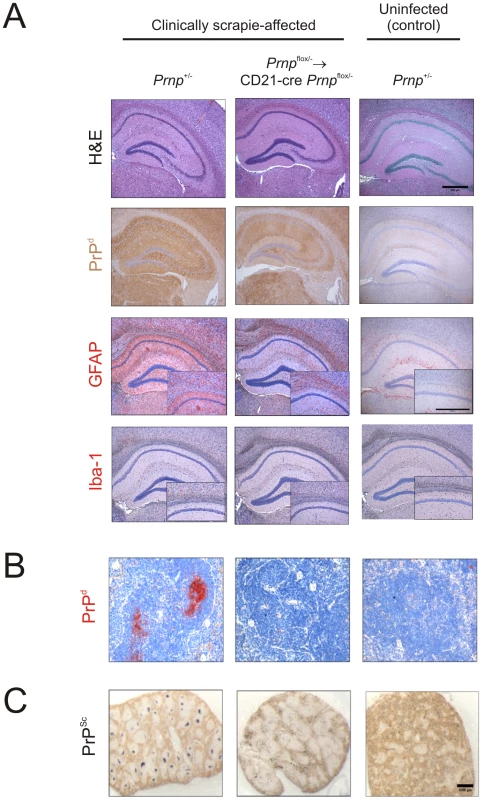
Control mice (Prnp+/- mice) and Prnpflox/-→CD21-Cre Prnpflox/- mice that lacked PrPC-expressing FDC were injected i.c. with the scrapie agent directly into the CNS. Brains and spleens were collected from clinically scrapie-affected mice to compare the neuropathology and cellular sites of PrPSc accumulation. A) High levels of spongiform pathology (H&E, upper row), heavy accumulations of PrPd (brown, second row), reactive astrocytes expressing GFAP (brown, third row) and active microglia expressing Iba-1 (brown, bottom row) were detected in the hippocampi of the brains of all clinically scrapie-affected mice. Scale bars, 500 µm. B) High levels of PrPd (red) were detected in association with FDC in spleens from clinically scrapie-affected control mice that contained PrPC-expressing FDC. C) PET blot analysis of analysis of adjacent sections by PET-immunoblot analysis confirmed the presence of PK-resistant PrPSc (blue/black). In contrast, no PrPd or PrPSc was detected in spleens of Prnpflox/-→CD21-Cre Prnpflox/- that lacked PrPC-expressing FDC. Scale bars = 500 µm. Effect of FDC-restricted PrPC-ablation prion neuroinvasion after i.p. exposure
Studies in mice show that efficient prion neuroinvasion from peripheral sites of exposure is dependent upon the presence of FDC in lymphoid tissues [1], [4], [35], [44]–[46]. Next, the effect of FDC-specific Prnp-ablation on prion neuroinvasion via the peritoneal route was determined. Unfortunately, due to the advanced ages of the mice in this experiment, some succumbed to ageing-related inter-current illness. As there was a 100 days interval between the time of lethal γ-irradiation/bone marrow reconstitution and prion infection, many mice were approximately 500–600 days old when culled. However, most mice with PrPC-expressing FDC in their spleens succumbed to clinical prion disease after i.p. injection (Prnp+/-→ Prnp+/- control mice, n = 5/7; CD21-Cre Prnpflox/-→Prnpflox/- mice, n = 3/6; Table S1). Histopathological analysis showed that brains from all clinically-affected mice from these groups displayed the characteristic spongiform pathology, astrogliosis, microgliosis and PrPd accumulation typically associated with terminal infection with the ME7 scrapie agent (Figure S3, third and fourth columns). In contrast, none of the mice with PrPC-ablated FDC (Prnpflox/-→CD21-Cre Prnpflox/- mice, n = 0/6; CD21-Cre Prnpflox/-→CD21-Cre Prnpflox/- mice, n = 0/7) succumbed to clinical prion disease during their life-spans (Table S1). Although we cannot exclude the possibility that if the clinically-negative mice with PrPC-ablated FDC mice had lived longer some may have succumbed to clinical prion disease after substantially extended incubation periods, no PrPd or other characteristic histopathological hallmarks of prion disease were detected in their brains (Figure S3, first two columns). Together, these data suggest that in the specific absence of PrPC expression on FDC neuroinvasion following peripheral exposure is impaired.
Discussion
These data definitively demonstrate that FDC are essential sites of prion replication in lymphoid tissues. In order to precisely establish the role of FDC in prion pathogenesis two unique compound transgenic mouse models were created in which PrPC expression was specifically “switched on” or “off” only on FDC. Our data confirm that FDC express high levels of PrPC and do not simply acquire it from other host cells. Furthermore, we show that following peripheral exposure PrPC-expressing FDC alone are sufficient to sustain high levels of prion replication in the spleen. Accordingly, when PrPC-expression was specifically ablated only on FDC prion replication in the spleen was blocked. These data likewise demonstrate that FDC do not simply acquire prions after their release from other infected host cells. Our analysis showed that the effects of Prnp-ablation on prion replication in the spleen were specific to FDC and had no effect on prion neuropathogenesis when the infection was established directly in the CNS. In the absence of PrPC expression on FDC the PrPSc from the initial inoculum appeared to be scavenged by tingible body macrophages resident within the B cell follicles. Together, these data definitively demonstrate that FDC are the critical early sites of prion replication in lymphoid tissues. This study is the first to demonstrate that the specific ablation of a cellular protein only on FDC, without apparent consequences for FDC status and function, blocks the replication of an important pathogen in the spleen.
FDC reside in the primary B cell follicles and germinal centres of lymphoid tissues and are a completely distinct cell lineage from bone-marrow-derived classical dendritic cells [47]–[49]. FDC possess many slender and convoluted dendritic processes which provide the FDC with an extremely large surface area. This helps the FDC to efficiently trap and retain large amounts of native antigen in the form of immune complexes, consisting of antigen-antibody and/or complement components. The longevity of FDC ensures that antigen is retained upon their surfaces for long periods [50], [51]. Antigens trapped on the surface of FDC are considered to promote immunoglobulin-isotype class switching, affinity maturation of naïve IgM+ B cells and the maintenance of immunological memory [38]–[42]. FDC are also considered to aid the clearance of apoptotic B lymphocytes [52], and play a role in infection with human immunodeficiency virus [53] and the pathogenesis of chronic inflammatory and autoimmune diseases [54] and peripherally-acquired prion infections.
A number of studies have addressed the role of FDC in prion pathogenesis. They show that prion replication in the spleen and subsequent neuroinvasion are both impaired in immunodeficient mice that lack FDC [4], [44], [45], or following their temporary de-differentiation [1], [35], [46]. Although the precise identity of FDC precursor cells is unknown, other studies have exploited their non-haematopoietic-origin to address their role in prion pathogenesis. In these bone marrow chimera studies, mismatches were created in Prnp expression between the FDC-containing stromal and haematopoietic compartments by grafting bone marrow cells from PrP-deficient (Prnp-/-) mice into PrP-expressing wild-type mice, and vice versa [13], [14]. Using this approach FDC and all other stromal cells were derived from the recipient, whereas lymphocytes and other haematopoietic lineages were derived from the donor cells. Following peripheral exposure prion accumulation upon FDC was only detected in the spleens of mice with a Prnp-expressing stromal compartment.
While the above studies clearly show that the presence of FDC is important for prion replication in the spleen, it was not possible to dissociate the Prnp expression status of FDC from that of the nervous system and all other non-haematopoietic host-cell populations and therefore precisely characterise the role of FDC in prion neuroinvasion [13], [14]. This is important for a number of reasons. Firstly, prion infection can occur within inflammatory PrPC-expressing stromal cells that are distinct from FDC [23]. Secondly, the FDC's ability to bind exosomes may have lead to the wrong interpretation to be made in earlier studies describing their ontology [55]. Most evidence indicates that FDC do not derive from haematopoietic precursors [29], [49]. However, the detection of donor bone marrow derived MHC class-I molecules, and other donor-derived antigens, on the surface of FDC in recipient mice was considered evidence of FDC precursor cells within bone marrow [55]. With hindsight these observations are most likely due to the FDC's capacity to acquire exosome-associated antigens from other cell types [21]. Both PrPC and PrPSc can be released from cells in association with exosomes [20]. The possibility, therefore, cannot be excluded that FDC passively acquire prions after their release in exosomes from other infected non-haematopoietic cell populations. Finally, FDC characteristically trap and retain immune complexes on their surfaces. FDC express negligible levels of complement component C4 at the mRNA level but the detection of abundant activated C4 on their surfaces by IHC using mAb FDC-M2 (as used in this study) is indicative of the capture and retention of immune complexes by FDC [32]. Opsonising complement components and cellular CR are likewise considered to play an important role in the retention of prions by FDC [15], [16], [18]. Thus FDC may simply act as concentrating depots for prion-containing complement-opsonized immune complexes.
The practical hurdles that are encountered when attempting to isolate highly purified FDC from lymphoid tissues have made detailed analysis of their pathobiological functions extremely difficult. The main issues include: contamination with other cell types such as B cells and tingible body macrophages which express MFGE8 (FDC-M1), a common marker used to identify FDC [52], [56], low yield, and their dependence on constitutive lymphotoxin β receptor-stimulation to maintain their differentiated state [57]. FDC and mature B cells express high levels of Cr2 which encodes the complement receptors CR2/CR1 (CD21/35) [18], [27]. A previous study used CD21-cre mice to study FDC-specific gene function [27]. In the current study, our data confirm that Cre/loxP-mediated DNA recombination was specific to FDC and mature B cells in CD21-cre mice, and could be restricted to FDC by transfusing the mice with Cre-deficient bone marrow. In some Cre transgenic mouse lines Cre-toxicity is encountered whereby Cre recombinase causes mis-recombination, DNA damage and death of Cre-expressing cells [30]. However, our analysis suggested no significant effect of Cre-expression on the number, size and status of FDC networks and B cell follicles. CD21-Cre mice are therefore a powerful in vivo tool in which to study FDC-specific gene expression and function.
Expression of PrPC is mandatory for host cells to sustain prion infection [43]. In the current study to establish whether FDC actively amplify prions a compound transgenic mouse model was created using the CD21-cre mouse line to specifically “switch on” PrPC expression only on FDC (Prnpstop/-→CD21-Cre Prnpstop/- mice). As a consequence, only FDC in these mice had the potential to be actively infected with and replicate prions. Our analysis showed that expression of PrPC only on FDC was sufficient to sustain high levels of PrPSc accumulation upon FDC in the spleen after peripheral prion exposure. These data definitively demonstrate that FDC are the critical sites of prion replication in lymphoid tissues. Ultrastructural analysis of the cellular compartments within which PrPd localizes upon/within FDC has failed to show any intracellular accumulation. Instead the PrPd appears to be restricted to the plasmalemma of their dendritic processes [58]. This implies that early de novo PrPSc conversion occurs upon the surface of FDC.
A second compound transgenic mouse model was created in which PrPC expression was specifically “switched off” only on FDC (Prnpflox/-→CD21-Cre Prnpflox/- mice). If, as shown above, FDC do actively amplify prions, then one would also expect the specific ablation of PrPC expression only on FDC to block prion replication in the spleen. Our data confirmed this to be the case. As PrPC expression in all other host cells (eg: neurones) in these mice was unaffected, these data clearly show that FDC do not simply acquire prions following release from other infected host cells, even in mice with clinical prion disease in the brain. IHC analysis implied that in the spleens of mice with PrP-deficient FDC the prions appeared to be scavenged by tingible body macrophages resident within the B cell follicles. The lack of detection of PrPd within tingible body macrophages in the spleens of clinically-affected mice with PrP-deficient FDC (Figure 9) clearly demonstrates that these cells are not alternative sites of replication of ME7 scrapie prions. High levels of prions rapidly accumulate within the spleen and other lymphoid tissues within weeks of peripheral exposure. The magnitude of the prion accumulation within the spleen rapidly reaches a plateau level which is maintained for the duration of the disease [13], [44]. The maintenance of this plateau may be the consequence of a competitive state whereby FDC act to amplify prions above the threshold required to achieve neuroinvasion, whereas phagocytic cells such as macrophages act to destroy them [59], [60]. Indeed increased numbers of PrPd-containing tingible body macrophages are found within the B cell follicles of TSE-affected animals [58]. Thus, our data suggest that in the specific absence of PrPC expression by FDC the initial inoculum is phagocytosed and gradually degraded by mononuclear phagocytes such as tingible body macrophages [59], [60]. These data are congruent with data from our earlier study which likewise occasionally detected trace levels of prions from the initial inoculum within tingible body macrophages in the spleens of mice with a PrPC-deficient FDC-containing stromal compartment [13].
The density of sympathetic nerves can significantly influence the amount of prion accumulation in the spleen [33]. In the current study the distribution of TH-positive sympathetic nerves in the spleens of the FDC-specific gene targeted mouse lines was not adversely affected. Furthermore, when prions were injected directly to the brain, FDC-specific Prnp ablation had no influence on the onset of clinical disease or the neuropathology. These data provide strong evidence that the effects of Cre-mediated Prnp ablation on prion replication in the spleen were specific to FDC and not due to unregulated ablation of PrPC expression within the nervous system. In the current study PrPSc accumulation upon PrPC-ablated FDC (Prnpflox/-→CD21-Cre Prnpflox/- mice) was blocked even in spleens from i.c. injected clinically-scrapie affected mice. These data contrast those reported by Crozet and colleagues [61] which used Tg(OvPrP4) mice that express the ovine PRNP gene under the control of the neuron-specific enolase promoter on a murine Prnp-/- background. As a consequence ovine PrPC is expressed only in neurones. In contrast to data in the current study, when Tg(OvPrP4) mice were injected i.c. with a high dose of natural sheep scrapie PrPSc was detected in the germinal centres of their spleens. The reasons for this discrepancy are uncertain. However, the expression of PrPC in the neuronal compartment of Tg(OvPrP4) mice is 2-4X higher than in controls. In the current study in mice in which PrPC was ablated only on FDC (Prnpflox/-→CD21-Cre Prnpflox/- mice) the expression of murine Prnp in Cre-deficient cells such as neurones is controlled by the endogenous Prnp promoter and expressed at similar levels to controls (Figure 5E). In the presence of increased PrPC expression on neurones it is plausible that greater prion replication occurred within the peripheral nervous system, which may have been subsequently trapped on the surface of the FDC and scavenged by macrophages as the prion burden increased. Similarly, hyper-innervation of the spleen likewise leads to increase prion burden in this tissue [33].
In conclusion, our data demonstrate that PrPC-expressing FDC are the essential sites of prion replication in lymphoid tissues. Indeed, PrPC-expression on FDC alone was sufficient to sustain high levels of prion replication. In contrast, the specific ablation of PrPC expression on FDC blocked prion replication. Although FDC have the capacity to bind exosomes and immune complexes which may contain PrPSc, this finding clearly demonstrates that FDC do not simply passively acquire prions from other infected cell populations such as neurones. Previous data show treatments which impair the status or immune complex-trapping function of FDC reduce prion susceptibility after peripheral exposure [1], [16], [35], [46], [62]. The demonstration that Prnp-ablation only on FDC blocked splenic prion replication without apparent consequences for FDC status represents a novel opportunity to prevent neuroinvasion by modulation of PrPC expression on FDC.
Materials and Methods
Ethics statement
All studies using experimental mice and regulatory licences were approved by both The Roslin Institute's and University of Edinburgh's Protocols and Ethics Committees. All animal experiments were carried out under the authority of a UK Home Office Project Licence within the terms and conditions of the strict regulations of the UK Home Office ‘Animals (scientific procedures) Act 1986'. Where necessary, anaesthesia appropriate for the procedure was administered, and all efforts were made to minimize harm and suffering. Mice were humanely culled using by a UK Home Office Schedule One method.
Mice
The CD21-Cre [26], ROSA26flox/flox reporter strain [28], Prnp-/- [12] mice and tga20 mice over-expressing PrPc [63] were generated as described previously. Prnpflox/flox mice have loxP sites flanking exon 3 of the Prnp gene [31]. Prnpstop/- mice have a floxed β-geo cassette inserted into intron 2 of the Prnp gene upstream of exon 3 [31]. Mice were maintained under SPF conditions.
Genotype confirmation by PCR analysis
Prior to their use in experiments, the genotype of each mouse was confirmed by PCR analysis. DNA was prepared from tails, blood and spleens using the DNeasy blood and tissue kit (Qiagen, Crawley, UK) according to the manufacturer's instructions. Where indicated DNA samples were analysed for presence of Cre, LacZ, Prnp+/+, Prnp-/-, Prnpflox, recombined Prnpflox (Prnpde-flox), Prnpstop and recombined Prnpstop (Prnpstop(R)) using the primers listed in Table 1. PCR products were resolved by electrophoresis through a 1.0% agarose gel containing 0.002% GelRed (Biotium, Cambridge Biosciences Ltd, Cambridge, UK).
Tab. 1. PCR primers used to confirm the genotypes of mice used in this study. 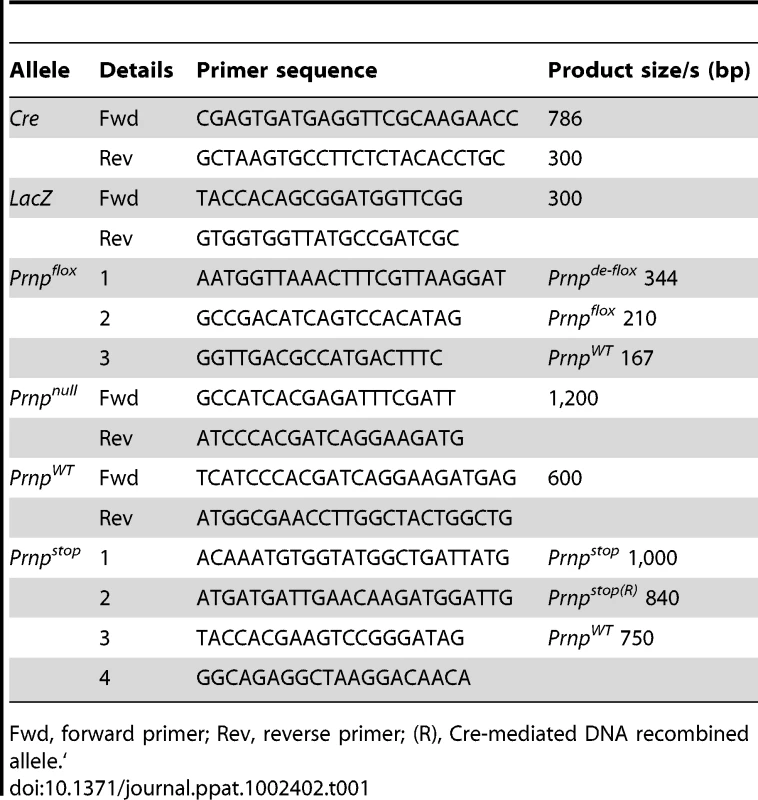
Fwd, forward primer; Rev, reverse primer; (R), Cre-mediated DNA recombined allele. γ-Irradiation and bone-marrow reconstitution
Bone-marrow from the femurs and tibias of donor mice was prepared as single-cell suspensions (3×107–4×107 viable cells/ml) in HBSS (Invitrogen, Paisley, UK). Recipient adult (6–8 weeks old) mice were γ-irradiated (950 rad) and 24 h later reconstituted with 100 µl bone-marrow by injection into the tail vein. Recipient mice were used in subsequent experiments as described 100 days after bone marrow reconstitution to allow sufficient time for removal of long-lived B lymphocyte populations and their replacement from the donor bone marrow.
Histological assessment of Lacz expression
Tissues were first immersed in LacZ fixative [PBS (pH 7.4) containing 2% paraformaldehyde, 0.2% gluteraldehyde, 0.02% Nonidet P40, 0.01% sodium deoxycholate, 5 mM EGTA, 2 mM MgCl2] and washed in LacZ wash buffer [PBS (pH 7.4) containing 0.02% Nonidet P40, 0.01% sodium deoxycholate, 2 mM MgCL2]. Tissues were subsequently incubated in 15% (wt/vol) sucrose in PBS overnight followed by a further overnight incubation in 30% (wt/vol) sucrose in PBS and embedded in Tissue-Tek O.C.T. compound (Bayer PLC, Newbury, UK). Serial sections (thickness 8 µm) were cut on cryostat and stained overnight at 37°C with LacZ staining solution (Glycosynth, Warrington, UK). Staining reaction was stopped by washing in LacZ wash buffer followed by dH2O. Sections were counterstained with nuclear fast red (Vector Laboratories, Peterborough, UK).
Prion exposure and disease monitoring
For i.c. or i.p. exposure mice were injected with 20 µl of a 1% (v/w) scrapie brain homogenate prepared from mice terminally-affected with ME7 scrapie prions (containing approximately 1×104 i.c. ID50 units). Following exposure, mice were coded and assessed blindly for signs of clinical disease and culled at a standard clinical endpoint [64]. Survival times were recorded for mice that did not develop clinical signs of disease and were culled when they showed signs of intercurrent disease. Scrapie diagnosis was confirmed blindly on coded sections by histopathological assessment of vacuolation in the brain. For the construction of lesion profiles, vacuolar changes were scored in nine grey-matter areas of brain as described [65]. Where indicated, some four mice from each group were culled at the times indicated post injection with scrapie and tissues taken for further analysis. For bioassay of scrapie agent infectivity, individual half spleens were prepared as 10% (wt/vol) homogenates in physiological saline. Groups of four tga20 indicator mice were injected i.c. with 20 µl of each homogenate. The scrapie titre in each sample was determined from the mean incubation period in the indicator mice, by reference to a dose/incubation period response curve for ME7 scrapie-infected spleen tissue serially titrated in tga20 mice using the relationship: y = 9.4533–0.0595x (y, = log ID50 U/20 µl of homogenate; x, incubation period; R2 = 0.9562). As the expression level of cellular PrPc controls the prion disease incubation period, tga20 mice overexpressing PrPc are extremely useful as indicator mice in prion infectivity bioassays as they succumb to disease with much shorter incubation times than conventional mouse strains [63].
IHC and immunofluorescent analyses
Spleens were removed and snap-frozen at the temperature of liquid nitrogen. Serial frozen sections (10 µm in thickness) were cut on a cryostat and immunostained with the following antibodies: FDCs were visualized by staining with mAb 7G6 to detect CR2/CR1 (CD21/CD35; BD Biosciences PharMingen), mAb FDC-M2 to detect C4 (AMS Biotechnology, Oxon, UK) or mAb 8C12 to detect CR1 (CD35; BD Biosciences PharMingen). Cellular PrPC was detected using PrP-specific polyclonal antibody (pAb) 1B3 [66]. B cells were detected using mAb B220 to detect CD45R (Caltag, Towcester, UK), or anti-CD19 (BD biosciences PharMingen). Marginal zone B cells were detected using mAb 1B1 to detect CD1d (BD Biosciences PharMingen). Sympathetic nerves were detected using tyrosine hydroxylase (TH)-specific pAb (Chemicon Europe).
For the detection of disease-specific PrP (PrPd) in spleens and brains, tissues were fixed in periodate-lysine-paraformaldehyde fixative and embedded in paraffin wax. Sections (thickness, 6 µm) were deparaffinised, and pre-treated to enhance the detection of PrPd by hydrated autoclaving (15 min, 121°C, hydration) and subsequent immersion formic acid (98%) for 5 min [67]. Sections were then immunostained with 1B3 PrP-specific pAb. For the detection of EGF-like module-containing mucin-like hormone receptor-like 1 (EMR1)-expressing macrophages, paraffin-embedded spleen sections were micro-waved in citric acid buffer (pH 6.0) for 10 min. Endogenous peroxidase activity was blocked using 1% hydrogen peroxidase in methanol, and macrophages detected using rat mAb F4/80 to detect EMR1 (clone CI:A3-1, AbD Serotec). For the detection of astrocytes, brain sections were immunostained with anti-glial fibrillary acidic protein (GFAP; DAKO, Ely, UK). For the detection of microglia, deparaffinised brain sections were first pre-treated with Target Retrieval Solution (DAKO) and subsequently immunostained with anti-ionized calcium-binding adaptor molecule 1 (Iba-1; Wako Chemicals GmbH, Neuss, Germany). Immunolabelling was revealed using HRP-conjugated to the avidin-biotin complex (Novared kit, Vector laboratories, Peterborough, UK). Paraffin-embedded tissue (PET) immunoblot analysis was used to confirm the PrPd detected by immunohistochemistry was proteinase K (PK)-resistant PrPSc [34]. Membranes were subsequently immunostained with 1B3 PrP-specific pAb.
For light microscopy, following the addition of primary antibodies, biotin-conjugated species-specific secondary antibodies (Stratech, Soham, UK) were applied followed by alkaline phosphatase or HRP coupled to the avidin/biotin complex (Vector Laboratories). Vector Red (Vector Laboratories) and diaminobenzidine (DAB; Sigma Aldrich, Dorset, UK) were used as substrates, respectively, and sections were counterstained with haematoxylin to distinguish cell nuclei. For fluorescent microscopy, following the addition of primary antibody, species-specific secondary antibodies coupled to Alexa Fluor 488 (green), Alexa Fluor 594 (red) dyes or Alexa Fluor 647 (blue) dyes (Invitrogen, Paisley, UK) were used. Sections were mounted in fluorescent mounting medium (DakoCytomation) and examined using a Zeiss LSM5 confocal microscope (Zeiss, Welwyn Garden City, UK).
Image analysis
Digital microscopy images were analyzed using ImageJ software (http://rsbweb.nih.gov/ij/) as described [68]. Intensity thresholds were first applied and then the number of pixels of each colour (black, red, green, yellow) were then automatically counted and presented as a proportion of the total number of pixels in each area under analysis. The preferential co-localisation of fluorochromes was determined by comparisons of the observed distribution of colours with those predicted by the null hypothesis that each element of positive staining was randomly and independently distributed. Values found to be significantly greater than the null hypothesis confirm significant co-localisation of fluorochromes. Spleens from 6 mice from each group were analyzed. From each spleen, 2 sections were studied and on each section data from 4 individual FDC networks collected. Thus, for each mouse group data from a total of 48 individual FDC were analysed. Similarly, data from 48 images from each group were analyzed to determine the preferential co-localisation of fluorochromes upon TH-positive sympathetic nerves within the spleen. A one-way ANOVA test was then used to compare the null hypothesis (that the pixels were randomly distributed) to the observed levels of co-localisation.
Passive immunization
To assess antigen trapping by FDC in vivo, mice were passively immunized by intravenous injection with 100 µl preformed PAP immune complexes (Sigma). Spleens were removed 24 h later and the presence of FDC-associated immune complexes identified by IHC.
Statistical analyses
Data are presented as mean ± SE. Unless indicated otherwise, significant differences between samples in different groups were sought by one-way ANOVA. Values of P<0.05 were accepted as significant.
Supporting Information
Zdroje
1. MabbottNAYoungJMcConnellIBruceME 2003 Follicular dendritic cell dedifferentiation by treatment with an inhibitor of the lymphotoxin pathway dramatically reduces scrapie susceptibility. J Virol 77 6845 6854
2. PrinzMHuberGMacphersonAJSHeppnerFLGlatzelM 2003 Oral prion infection requires normal numbers of Peyer's patches but not of enteric lymphocytes. Am J Pathol 162 1103 1111
3. HoriuchiMFuruokaHKitamuraNShinagawaM 2006 Alymphoplasia mice are resistant to prion infection via oral route. Jap J Vet Res 53 149 157
4. GlaysherBRMabbottNA 2007 Role of the GALT in scrapie agent neuroinvasion from the intestine. J Immunol 178 3757 3766
5. AndreolettiOBerthonPMarcDSarradinPGrosclaudeJ 2000 Early accumulation of PrPSc in gut-associated lymphoid and nervous tissues of susceptible sheep from a Romanov flock with natural scrapie. J Gen Virol 81 3115 3126
6. SigurdsonCJWilliamsESMillerMWSprakerTRO'RourkeKI 1999 Oral transmission and early lymphoid tropism of chronic wasting disease PrPres in mule deer fawns (Odocoileus hemionus). J Gen Viroly 80 2757 2764
7. HiltonDFathersEEdwardsPIronsideJZajicekJ 1998 Prion immunoreactivity in appendix before clinical onset of variant Creutzfeldt-Jakob disease. Lancet 352 703 704
8. WilkeGSteinhauserGGrunJBerekC 2010 In silico subtraction approach reveals a close lineage relationship between follicular dendritic cells and BP3hi stromal cells isolated from SCID mice. Eur J Immunol 40 2165 2173
9. BeekesMMcBridePA 2007 The spread of prions through the body in naturally acquired transmissible spongiform encephalopathies. FEBS J 274 588 605
10. BoltonDCMcKinleyMPPrusinerSB 1982 Identification of a protein that purifies with the scrapie prion. Science 218 1309 1311
11. LegnameGBaskakovIVNguyenH-OBRiesnerDCohenFE 2004 Synthetic mammalian prions. Science 305 673 676
12. MansonJCClarkeARHooperMLAitchisonLMcConnellI 1994 129/Ola mice carrying a null mutation in PrP that abolishes mRNA production are developmentally normal. Mol Neurobiol 8 121 127
13. BrownKLStewartKRitchieDMabbottNAWilliamsA 1999 Scrapie replication in lymphoid tissues depends on PrP-expressing follicular dendritic cells. Nat Med 5 1308 1312
14. KleinMAFriggRRaeberAJFlechsigEHegyiI 1998 PrP expression in B lymphocytes is not required for prion neuroinvasion. Nat Med 4 1429 1433
15. KleinMAKaeserPSSchwarzPWeydHXenariosI 2001 Complement facilitates early prion pathogenesis. Nat Med 7 488 492
16. MabbottNABruceMEBottoMWalportMJPepysMB 2001 Temporary depletion of complement component C3 or genetic deficiency of C1q significantly delays onset of scrapie. Nat Med 7 485 487
17. MabbottNABruceME 2004 Complement component C5 is not involved in scrapie pathogenesis. Immunobiology 209 545 549
18. ZabelMDHeikenwalderMPrinzMArrighiISchwarzP 2007 Stromal complement receptor CD21/35 facilitates lymphoid prion colonization and pathogenesis. J Immunol 179 6144 6152
19. DenzerKKleijmeerMJHeijnenHFGStoorvogelWGeuzeHJ 2000 Exosome: from internal vesicle of the multivesicular body to intercellular signalling device. J Cell Sci 113 3365 3374
20. FevrierBViletteDArcherFLoewDFaigleW 2004 Cells release prions in association with exosomes. Proc Natl Acad Sci USA 101 9683 9688
21. DenzerKvan EijkMKleijmeerMJJakobsonEde GrootC 2000 Follicular dendritic cells carry MHC class II-expressing microvesicles at their surface. J Immunol 165 1259 1265
22. MohanJBrownKLFarquharCFBruceMEMabbottNA 2004 Scrapie transmission following exposure through the skin is dependent on follicular dendritic cells in lymphoid tissues. J Dermatol Sci 35 101 111
23. HeikenwalderMKurrerMOMargalithIKranichJZellerN 2008 Lymphotoxin-dependent prion replication in inflammatory stromal cells of granulomas. Immunity 29 998 1008
24. ThomzigAKratzelCLenzGKrügerDBeekesM 2003 Widespread PrPSc accumulation in muscles of hamsters orally infected with scrapie. EMBO Rep 4 530 533
25. ŠimákJHolandaKD'AgnilloFJanotaJVostalJG 2002 Cellular prion protein in expressed on endothelial cells and is released during apoptosis on membrane microparticles found in human plasma. Transfusion 42 334 342
26. KrausMAlimzhanovMBRajewskyNRajewskyK 2004 Survival of resting mature B lymphocytes depends on BCR signaling via the Igα/β heterodimer. Cell 117 787 800
27. VictoratosPLagnelJTzimaSAlimzhanovMBRajewskyK 2006 FDC-specific functions of p55TNFR and IKK2 in the development of FDC networks and of antibody responses. Immunity 24 65 77
28. MaoXFujiwaraYOrkinSH 1999 Improved reporter strain for monitoring Cre recombinase-mediated DNA excisions in mice. Proc Natl Acad Sci, USA 96 5037 5042
29. TkachukMBolligerSRyffelBPluschkeGBanksTA 1998 Crucial role of tumour necrosis factor receptor 1 expression on nonhematopoietic cells for B cell localization within the splenic white pulp. J Exp Med 187 469 477
30. Schmidt-SupprianMRajewskyK 2007 Vagaries of conditional gene targeting. Nat Immunol 8 665 668
31. TuziNLClarkeARBradfordBAitchisonLThomsonV 2004 Cre-loxP mediated control of PrP to study transmissible spongiform encephalopathy diseases. Genesis 40 1 6
32. TaylorPRPickeringMCKosco-VilboisMHWalportMJBottoM 2002 The follicular dendritic cell restricted epitope, FDC-M2, is complement C4; localization of immune complexes in mouse tissues. Eur J Immunol 32 1883 1896
33. GlatzelMHeppnerFLAlbersKMAguzziA 2001 Sympathetic innervation of lymphoreticular organs is rate limiting for prion neuroinvasion. Neuron 31 25 34
34. Schulz-SchaefferWJTschokeSKranefussNDroseWHause-ReitnerD 2000 The paraffin-embedded tissue blot detects PrPsc early in the incubation time in prion diseases. Am J Pathol 156 51 56
35. MabbottNAMackayFMinnsFBruceME 2000 Temporary inactivation of follicular dendritic cells delays neuroinvasion of scrapie. Nat Med 6 719 720
36. RaymondCRAucouturierPMabbottNA 2007 In vivo depletion of CD11c+ cells impairs scrapie agent neuroinvasion from the intestine. J Immunol 179 7758 7766
37. BrownKLWathneGJSalesJBruceMEMabbottNA 2009 The effects of host age on follicular dendritic cell status dramatically impair scrapie agent neuroinvasion in aged mice. J Immunol 183 5199 5207
38. FuY-XMolinaHMatsumotoMHuangGMinJ 1997 Lymphotoxin-α (LTα) supports development of splenic follicular structure that is required for IgG response. J Exp Med 185 2111 2120
39. FuY-XHuangGWangYChaplinDD 1998 B lymphocytes induce the formation of follicular dendritic cell clusters in a lymphotoxin α-dependent fashion. J Exp Med 187 1009 1018
40. EndresRAlimzhanovMBPlitzTFuttererAKosco-VilboisMH 1999 Mature follicular dendritic cell networks depend on expression of lymphotoxin β receptor by radioresistant stromal cells and of lymphotoxin β and tumour necrosis factor by B cells. J Exp Med 189 159 168
41. FuY-XHuangGWangYChaplinDD 2000 Lymphotoxin-α-dependent spleen microenvironment supports the generation of memory B cells and is required for their subsequent antigen-induced activation. J Immunol 164 2508 2514
42. AydarYSukumarASzakalAKTewJG 2005 The influence of immune complex-bearing follicular dendritic cells on the IgM response, Ig class switching, and production of high affinity IgG. J Immunol 174 5358 5366
43. MansonJCClarkeARMcBridePAMcConnellIHopeJ 1994 PrP gene dosage determines the timing but not the final intensity or distribution of lesions in scrapie pathology. Neurodegeneration 3 331 340
44. MabbottNAWilliamsAFarquharCFPasparakisMKolliasG 2000 Tumor necrosis factor-alpha-deficient, but not interleukin-6-deficient, mice resist peripheral infection with scrapie. J Virol 74 3338 3344
45. PrinzMMontrasioFKleinMASchwarzPPrillerJ 2002 Lymph nodal prion replication and neuroinvasion in mice devoid of follicular dendritic cells. Proc Natl Acad Sci USA 99 919 924
46. MontrasioFFriggRGlatzelMKleinMAMackayF 2000 Impaired prion replication in spleens of mice lacking functional follicular dendritic cells. Science 288 1257 1259
47. ShortmanKLiuY-J 2002 Mouse and human dendritic cell subtypes. Nat Rev Immunol 2 151 161
48. ImazekiNSenooAFuseY 1992 Is the Follicular Dendritic Cell a Primarily Stationary Cell? Immunology 76 508 510
49. MabbottNABailieJKKobayashiADonaldsonDSOhmoriH 2011 Expression of mesenchyme-specific gene signatures by follicular dendritic cells: insights from the meta-analysis of microarray data from multiple mouse cell populations. Immunology 133 482 498
50. MandelTEPhippsRPAbbotATewJG 1980 The follicular dendritic cell: long term antigen retention during immunity. Immunol Review 53 29 59
51. SuzukiKGrigorovaIPhanTGKellyLMCysterJG 2009 Visualizing B cell capture of cognate antigen from follicular dendritic cells. J Exp Med 206 1485 1493
52. KranichJKrautlerNJHeinenEPolymenidouMBridelC 2008 Follicular dendritic cells control engulfment of apoptotic bodies by secreting Mfge8. J Exp Med 205 1293 1302
53. BurtonGFBrandonFKEstesJDThackerTCGartnerS 2002 Follicular dendritic cell contributions to HIV pathogenesis. Sem Immunol 14 275 284
54. GommermanJLBrowningJL 2003 Lymphotoxin/LIGHT, lymphoid microenvironments and autoimmune disease. Nat Rev Immunol 3 642 654
55. KapasiZFQinDKerrWGKosco-VilboisMHSchultzLD 1998 Follicular dendritic cell (FDC) precursors in primary lymphoid tissues. J Immunol 160 1078 1084
56. HanamayaRTanakaMMiyasakaKAozasaKKoikeM 2004 Autoimmune disease and impaired uptake of apoptotic cells in MFG-E8-deficient mice. Science 304 1147 1150
57. MackayFBrowningJL 1998 Turning off follicular dendritic cells. Nature 395 26 27
58. McGovernGMabbottNAJeffreyM 2009 Scrapie affects the maturation cycle and immune complex trapping by follicular dendritic cells in mice. PLoS One 4 e8186
59. CarpRICallahanSM 1982 Effect of mouse peritoneal macrophages on scrapie infectivity during extended in vitro incubation. Intervirology 17 201 207
60. MaignienTShakwehMCalvoPMarcéDSalèsN 2005 Role of gut macrophages in mice orally contaminated with scrapie or BSE. Int J Pharmaceutics 298 293 304
61. CrozetCLezmiSFlamantFSamarutJBaronT 2007 Peripheral circulation of the prion infectious agent in transgenic mice expressing the ovine prion protein in neurons only. J Infect Dis 195 997 1006
62. MohanJBruceMEMabbottNA 2005 Follicular dendritic cell dedifferentiation reduces scrapie susceptibility following inoculation via the skin. Immunology 114 225 234
63. FischerMRulickeTRaeberASailerAMoserM 1996 Prion protein (PrP) with amino-proximal deletions restoring susceptibility of PrP knockout mice to scrapie. EMBO J 15 1255 1264
64. FraserHDickinsonAG 1973 Agent-strain differences in the distribution and intensity of grey matter vacuolation. J Comp Pathol 83 29 40
65. FraserHDickinsonAG 1968 The sequential development of the brain lesions of scrapie in three strains of mice. J Comp Pathol 78 301 311
66. FarquharCFSomervilleRARitchieLA 1989 Post-mortem immunodiagnosis of scrapie and bovine spongiform encephalopathy. J Virol Met 24 215 222
67. McBridePEikelenboomPKraalGFraserHBruceME 1992 PrP protein is associated with follicular dendritic cells of spleens and lymph nodes in uninfected and scrapie-infected mice. J Pathol 168 413 418
68. InmanCFReesLENBarkerEHaversonKStokesCR 2005 Validation of computer-assisted, pixel-based analysis of multiple-colour immunofluorescence histology. J Immunoll Met 302 156 167
Štítky
Hygiena a epidemiologie Infekční lékařství Laboratoř
Článek Genesis of Mammalian Prions: From Non-infectious Amyloid Fibrils to a Transmissible Prion DiseaseČlánek Role of Permissive Neuraminidase Mutations in Influenza A/Brisbane/59/2007-like (H1N1) VirusesČlánek Allelic Variation on Murine Chromosome 11 Modifies Host Inflammatory Responses and Resistance toČlánek Multifaceted Regulation of Translational Readthrough by RNA Replication Elements in a TombusvirusČlánek Latent KSHV Infection of Endothelial Cells Induces Integrin Beta3 to Activate Angiogenic PhenotypesČlánek Controlling Viral Immuno-Inflammatory Lesions by Modulating Aryl Hydrocarbon Receptor Signaling
Článek vyšel v časopisePLOS Pathogens
Nejčtenější tento týden
2011 Číslo 12- Jak souvisí postcovidový syndrom s poškozením mozku?
- Měli bychom postcovidový syndrom léčit antidepresivy?
- Farmakovigilanční studie perorálních antivirotik indikovaných v léčbě COVID-19
- 10 bodů k očkování proti COVID-19: stanovisko České společnosti alergologie a klinické imunologie ČLS JEP
-
Všechny články tohoto čísla
- Inhibition of Apoptosis and NF-κB Activation by Vaccinia Protein N1 Occur via Distinct Binding Surfaces and Make Different Contributions to Virulence
- Genesis of Mammalian Prions: From Non-infectious Amyloid Fibrils to a Transmissible Prion Disease
- Kaposi's Sarcoma Herpesvirus microRNAs Target Caspase 3 and Regulate Apoptosis
- Nutritional Immunology: A Multi-Dimensional Approach
- Role of Permissive Neuraminidase Mutations in Influenza A/Brisbane/59/2007-like (H1N1) Viruses
- Vaccinomics and Personalized Vaccinology: Is Science Leading Us Toward a New Path of Directed Vaccine Development and Discovery?
- Symbiont Infections Induce Strong Cytoplasmic Incompatibility in the Tsetse Fly
- Allelic Variation on Murine Chromosome 11 Modifies Host Inflammatory Responses and Resistance to
- Computational and Biochemical Analysis of the Effector AvrBs2 and Its Role in the Modulation of Type Three Effector Delivery
- Granzyme B Inhibits Vaccinia Virus Production through Proteolytic Cleavage of Eukaryotic Initiation Factor 4 Gamma 3
- Association of Activating KIR Copy Number Variation of NK Cells with Containment of SIV Replication in Rhesus Monkeys
- Fungal Virulence and Development Is Regulated by Alternative Pre-mRNA 3′End Processing in
- versus the Host: Remodeling of the Bacterial Outer Membrane Is Required for Survival in the Gastric Mucosa
- Follicular Dendritic Cell-Specific Prion Protein (PrP) Expression Alone Is Sufficient to Sustain Prion Infection in the Spleen
- Autophagy Protein Atg3 is Essential for Maintaining Mitochondrial Integrity and for Normal Intracellular Development of Tachyzoites
- Longevity and Composition of Cellular Immune Responses Following Experimental Malaria Infection in Humans
- Sequential Adaptive Mutations Enhance Efficient Vector Switching by Chikungunya Virus and Its Epidemic Emergence
- Acquisition of Pneumococci Specific Effector and Regulatory Cd4 T Cells Localising within Human Upper Respiratory-Tract Mucosal Lymphoid Tissue
- The Meaning of Death: Evolution and Ecology of Apoptosis in Protozoan Parasites
- Deficiency of a Niemann-Pick, Type C1-related Protein in Is Associated with Multiple Lipidoses and Increased Pathogenicity
- Feeding Cells Induced by Phytoparasitic Nematodes Require γ-Tubulin Ring Complex for Microtubule Reorganization
- Eight RGS and RGS-like Proteins Orchestrate Growth, Differentiation, and Pathogenicity of
- Prion Uptake in the Gut: Identification of the First Uptake and Replication Sites
- Nef Decreases HIV-1 Sensitivity to Neutralizing Antibodies that Target the Membrane-proximal External Region of TMgp41
- Multifaceted Regulation of Translational Readthrough by RNA Replication Elements in a Tombusvirus
- A Temporal Role Of Type I Interferon Signaling in CD8 T Cell Maturation during Acute West Nile Virus Infection
- The Membrane Fusion Step of Vaccinia Virus Entry Is Cooperatively Mediated by Multiple Viral Proteins and Host Cell Components
- HIV-1 Capsid-Cyclophilin Interactions Determine Nuclear Import Pathway, Integration Targeting and Replication Efficiency
- Neonatal CD8 T-cell Hierarchy Is Distinct from Adults and Is Influenced by Intrinsic T cell Properties in Respiratory Syncytial Virus Infected Mice
- Two Novel Transcriptional Regulators Are Essential for Infection-related Morphogenesis and Pathogenicity of the Rice Blast Fungus
- Five Questions about Non-Mevalonate Isoprenoid Biosynthesis
- The Human Cytomegalovirus UL11 Protein Interacts with the Receptor Tyrosine Phosphatase CD45, Resulting in Functional Paralysis of T Cells
- Wall Teichoic Acids of Limit Recognition by the Drosophila Peptidoglycan Recognition Protein-SA to Promote Pathogenicity
- A Novel Role for the NLRC4 Inflammasome in Mucosal Defenses against the Fungal Pathogen
- Inflammasome-dependent Pyroptosis and IL-18 Protect against Lung Infection while IL-1β Is Deleterious
- CNS Recruitment of CD8+ T Lymphocytes Specific for a Peripheral Virus Infection Triggers Neuropathogenesis during Polymicrobial Challenge
- Latent KSHV Infection of Endothelial Cells Induces Integrin Beta3 to Activate Angiogenic Phenotypes
- A Receptor-based Switch that Regulates Anthrax Toxin Pore Formation
- Targeting of Heparin-Binding Hemagglutinin to Mitochondria in Macrophages
- Chikungunya Virus Neutralization Antigens and Direct Cell-to-Cell Transmission Are Revealed by Human Antibody-Escape Mutants
- Ce-Duox1/BLI-3 Generated Reactive Oxygen Species Trigger Protective SKN-1 Activity via p38 MAPK Signaling during Infection in
- Structural Elucidation and Functional Characterization of the Effector Protein ATR13
- Controlling Viral Immuno-Inflammatory Lesions by Modulating Aryl Hydrocarbon Receptor Signaling
- SAMHD1-Deficient CD14+ Cells from Individuals with Aicardi-Goutières Syndrome Are Highly Susceptible to HIV-1 Infection
- Acid Stability of the Hemagglutinin Protein Regulates H5N1 Influenza Virus Pathogenicity
- Cryo Electron Tomography of Herpes Simplex Virus during Axonal Transport and Secondary Envelopment in Primary Neurons
- A Novel Human Cytomegalovirus Locus Modulates Cell Type-Specific Outcomes of Infection
- Juxtamembrane Shedding of AMA1 Is Sequence Independent and Essential, and Helps Evade Invasion-Inhibitory Antibodies
- Pathogenesis and Host Response in Syrian Hamsters following Intranasal Infection with Andes Virus
- IRGM Is a Common Target of RNA Viruses that Subvert the Autophagy Network
- Epstein-Barr Virus Evades CD4 T Cell Responses in Lytic Cycle through BZLF1-mediated Downregulation of CD74 and the Cooperation of vBcl-2
- Quantitative Multicolor Super-Resolution Microscopy Reveals Tetherin HIV-1 Interaction
- Late Repression of NF-κB Activity by Invasive but Not Non-Invasive Meningococcal Isolates Is Required to Display Apoptosis of Epithelial Cells
- Polar Flagellar Biosynthesis and a Regulator of Flagellar Number Influence Spatial Parameters of Cell Division in
- Epstein-Barr Virus Nuclear Antigen 3C Stabilizes Gemin3 to Block p53-mediated Apoptosis
- The Enteropathogenic (EPEC) Tir Effector Inhibits NF-κB Activity by Targeting TNFα Receptor-Associated Factors
- Toward an Integrated Model of Capsule Regulation in
- A Systematic Screen to Discover and Analyze Apicoplast Proteins Identifies a Conserved and Essential Protein Import Factor
- A Host Small GTP-binding Protein ARL8 Plays Crucial Roles in Tobamovirus RNA Replication
- Comparative Pathobiology of Fungal Pathogens of Plants and Animals
- Synergistic Roles of Eukaryotic Translation Elongation Factors 1Bγ and 1A in Stimulation of Tombusvirus Minus-Strand Synthesis
- Engineered Immunity to Infection
- Inflammatory Monocytes and Neutrophils Are Licensed to Kill during Memory Responses
- Sialidases Affect the Host Cell Adherence and Epsilon Toxin-Induced Cytotoxicity of Type D Strain CN3718
- Eurasian-Origin Gene Segments Contribute to the Transmissibility, Aerosol Release, and Morphology of the 2009 Pandemic H1N1 Influenza Virus
- SARS Coronavirus nsp1 Protein Induces Template-Dependent Endonucleolytic Cleavage of mRNAs: Viral mRNAs Are Resistant to nsp1-Induced RNA Cleavage
- Identification and Characterization of a Novel Non-Structural Protein of Bluetongue Virus
- Functional Analysis of the Kinome of the Wheat Scab Fungus
- Norovirus Regulation of the Innate Immune Response and Apoptosis Occurs via the Product of the Alternative Open Reading Frame 4
- PLOS Pathogens
- Archiv čísel
- Aktuální číslo
- Informace o časopisu
Nejčtenější v tomto čísle- Controlling Viral Immuno-Inflammatory Lesions by Modulating Aryl Hydrocarbon Receptor Signaling
- Fungal Virulence and Development Is Regulated by Alternative Pre-mRNA 3′End Processing in
- Epstein-Barr Virus Nuclear Antigen 3C Stabilizes Gemin3 to Block p53-mediated Apoptosis
- Engineered Immunity to Infection
Kurzy
Zvyšte si kvalifikaci online z pohodlí domova
Současné možnosti léčby obezity
nový kurzAutoři: MUDr. Martin Hrubý
Všechny kurzyPřihlášení#ADS_BOTTOM_SCRIPTS#Zapomenuté hesloZadejte e-mailovou adresu, se kterou jste vytvářel(a) účet, budou Vám na ni zaslány informace k nastavení nového hesla.
- Vzdělávání



